Covid-19 vaccination: Is the world winning the war?
Covid-19 vaccination: Is the world winning the war?
Today some countries are progressing more rapidly than others in terms of covid-19 vaccinations. In this article, we will look at the cases of Israel, the UAE, and Morocco, and how successfully they have administered their inoculation campaigns. Then we will cover the issue of vaccine access inequality, and the reasons behind the gap between various nations.
Countries with the most successful and rapid vaccine rollout are the smaller ones in terms of population: Israel, UAE, etc. These countries’ advanced digitized and centralized healthcare systems allow for a quick and effective roll-out.
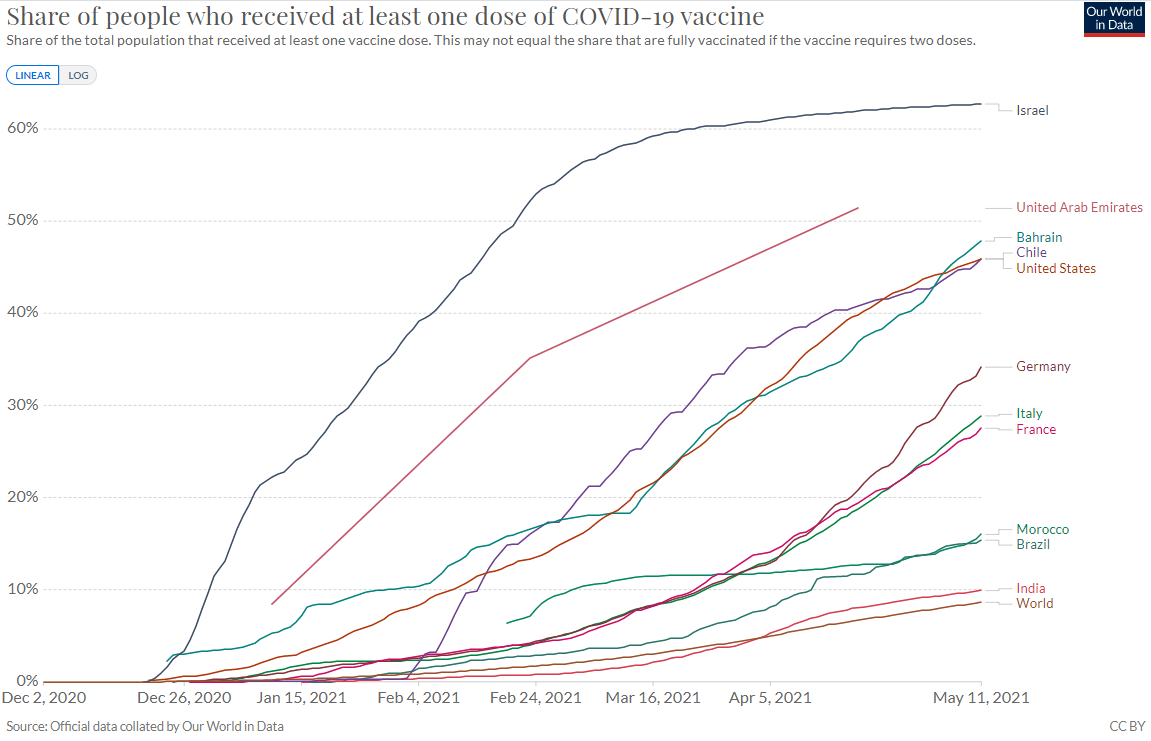
With a Covid-19 vaccination drive that has reached more than half of the population, Israel has pulled far ahead of the rest of the world, becoming a world leader in vaccinations per capita, and in return, it supplies BioNTech/Pfizer with valuable data and information from its campaign.
 Israel has started to reopen its economy since the Health Ministry data showed that the two-shot regimen has reduced COVID-19 infections by 95.8% since February and that it was 98% effective in preventing fever and breathing issues and 98.9% in preventing hospitalizations and death.
Israel has started to reopen its economy since the Health Ministry data showed that the two-shot regimen has reduced COVID-19 infections by 95.8% since February and that it was 98% effective in preventing fever and breathing issues and 98.9% in preventing hospitalizations and death.
In the UAE, Dubai has also decided to take the risk of gradually reopening its economy on New Year’s Eve, as it relies on international tourism for nearly a third of its GDP; by the end of January, with coronavirus cases spiking, hospitals had reached their limit and cases quadrupled to almost 4,000 a day.
The currently approved vaccines in the country are Sinopharm, Pfizer/BioNTech, and Sputnik V. The Emirates are one of the first countries to start vaccinations, having administered at least 11 million shots as of May 9th. Thanks to this early action, the economy of the UAE, is forecast to grow by 1.3% this year according to the IMF, after contracting 6.6% in 2020.
In Morocco, the vaccination campaign started on January 28th and has benefited some 4.5 million people (fully vaccinated), making it the most advanced African country in Covid-19 vaccinations. It currently uses the British AstraZeneca and Chinese Sinopharm vaccines and intends to further diversify its supplies with the Russian vaccine Sputnik V.
The Kingdom is emerging as a model country that seeks to vaccinate, free of charge, 80% of its population aged over 17, including foreign residents. On March 3rd, The World Health Organization congratulated Morocco and announced that it is among the first 10 countries that have “successfully completed the challenge of vaccination against COVID-19.”
Success of the Covid-19 vaccination campaign
One of the key factors of the success of the Covid-19 vaccination rollout is the population’s attitude towards it. Both the UAE and Israel have invested resources in reassuring their population that the vaccine is effective and safe. In many countries, health authorities relied on faith leaders to make sure their communities are getting their vaccines. In the UAE the Fatwa Council issued a Fatwa (Islamic ruling) allowing the Covid-19 vaccines to be used in compliance with Islamic Sharia’s objectives, and its chairman, Shaykh Abdallah bin Bayyah, was vaccinated in public.
Religious leaders are also spreading the word in Israel: ultra-Orthodox media and community leaders are taking part in the vaccination campaign, as a significant minority is still resistant and suspicious of the mass vaccination campaign.
In Morocco, the government has successfully managed the response to the pandemic by acting quickly and preemptively as the first cases appeared: through strict application of quarantine, acquisition of masks, and all the necessary PPE, early involvement in vaccination, and securing multiple doses of the vaccine. This effort has reduced the number of fatalities per day, from 92 deaths in November to only 5 in April.
How fair and equitable is the vaccine distribution plan?
So far, the richest countries have been prioritizing their own population and have been able to buy far more doses than the poorest ones: high-income countries hold a confirmed 4.2 billion doses, while low-middle income nations only hold 670 million.

In Africa, the delay appears to be playing out across the continent, which raised doubts about the effectiveness of political leadership. The delayed arrival of doses in some African nations could regrettably add more hospitalizations and deaths and increases the risk of multiplication of dangerous variants.
Led by the WHO with the Coalition for Epidemic Preparedness Innovations CEPI and Global Vaccine Alliance GAVI, the Covax initiative is aiming to focus on the 92 poorest countries: more than 49 million vaccine doses have been delivered through Covax so far. The World Health Organization approved the AstraZeneca vaccine to be rolled out globally through the Covax program and Ghana became the first to receive the Covid-19 vaccines in February.
A country with no vaccination plans: Tanzania
For months in 2020 the Tanzanian government, then led by the late John Magafuli, has insisted the country was “Covid-19 free”. And without providing any evidence, the government also expressed doubt about the efficacy of Covid-19 vaccines and instead promoted unfounded remedies like steam inhalation and herbal medicines, neither of which have been approved by the WHO. The health minister even went so far as to announce that the country “has no plans in place to accept COVID-19 vaccines”.
The deceased President opted to maintain strict control over public discussions of Covid-19 issuing a directive that only himself, Dr. Gwajima, and three other top officials could give information about Covid-19 in the country. But in an unusual move, some leaders of the Catholic church broke their silence and warned the public to observe health measures to prevent the spread of the virus.
WHO’s Africa director Dr. Matshidiso Moeti said that the vaccines work and that he encourages the Tanzanian government to prepare a Covid-19 vaccination campaign, adding that the WHO is ready to support them.
As the country has not published any data on the virus for months, it is difficult to say how well Tanzania’s approach has worked; the last time the country published data on its Covid-19 numbers was 29 April 2020, when it reported only 509 cases.
Why are such disparities allowed?
Since Covid-19 vaccines are not a public good, the market decides who gets it first. Wealthy countries are racing to have their population vaccinated this year, but in most developing and poor countries, the vaccine remains unavailable, undermining the efforts for global immunization.
The choices made by the wealthiest nations will determine which future takes hold: a global community unified to bring the virus under control, or a world divided between the wealthy and immunized and the vulnerable and poor.
Boutaina Benaboud
Sources:
https://covid19.ncema.gov.ae/en/page/about-the-vaccine
https://datadashboard.health.gov.il/COVID-19/general?utm_source=go.gov.il&utm_medium=referral
https://ourworldindata.org/covid-vaccinations
https://www.imf.org/en/Countries/ARE
https://www.bbc.com/news/world-55795297
https://www.eiu.com/n/85-poor-countries-will-not-have-access-to-coronavirus-vaccines/
https://twitter.com/omsmaroc?lang=en
https://www.mapnews.ma/en/actualites/social/covid-19-morocco-champion-vaccination-french-media








